Are you a new member? Sign up now
Login area
| Sign up
Blood Transfusion
I.Information For The Public
I. General Information1. The Blood
Blood is made up of cells (red blood cells, platelets and white blood cells) in a protein-rich liquid (plasma). Whole blood is almost never transfused to a patient; only the blood component needed is given to the patient.
2. Who Does my Donation Help?
Every 4 minutes someone in Lebanon needs blood. Half of all Lebanese will either need blood or know someone who will need blood at some point in their lives. It may be following an accident, during surgery or to support the treatment of an illness. By donating blood you may help a woman who has bled during childbirth, you may support the recovery of a cancer patient receiving chemotherapy; you may help people suffering from blood diseases during their treatment…
400 donations per day are needed.
Donating blood also allows you to:
2. Who Does my Donation Help?
Every 4 minutes someone in Lebanon needs blood. Half of all Lebanese will either need blood or know someone who will need blood at some point in their lives. It may be following an accident, during surgery or to support the treatment of an illness. By donating blood you may help a woman who has bled during childbirth, you may support the recovery of a cancer patient receiving chemotherapy; you may help people suffering from blood diseases during their treatment…
400 donations per day are needed.
Donating blood also allows you to:
- know your blood type
- have systematic biological testing (Hb/Ht count, serological testing…)
3. Blood Components
Today, with modern medical treatments, patient receive the specific blood component required in their particular condition. Up to four components can be derived from donated whole blood. This approach to treatment, referred to as blood component therapy, allows several patients to benefit from one unit of donated whole blood.
The main blood components include:
Today, with modern medical treatments, patient receive the specific blood component required in their particular condition. Up to four components can be derived from donated whole blood. This approach to treatment, referred to as blood component therapy, allows several patients to benefit from one unit of donated whole blood.
The main blood components include:
- Red cells, or erythrocytes, carry oxygen from the lungs to your body’s tissue and take carbon dioxide back to your lungs to be exhaled. They are routinely used for patients with massive hemorrhages or diseases causing severe or chronic anemias. They have a 42-day shelf life at 2-6 °C.
- Platelets, or thrombocytes, are small, colorless cell fragments in the blood whose main function is to interact with clotting proteins to stop or prevent bleeding.Platelets are given to patients who are not capable to produce sufficient platelet count in the bone marrow due to the disease or treatment process: patients with leukemia or bone marrow aplasia, patients receiving chemotherapy or radiation.
- Plasma is a fluid, composed of about 92% water, 7% vital proteins such as albumin, gamma globulin, anti- hemophilic factor, and other clotting factors, and 1% mineral salts, sugars, fats, hormones and vitamins. After donation plasma is frozen at -25°C and stored up to one year. Plasma is used to treat severely burned or injured patients. It is also given to patients with severe hemorrhages and coagulation disorders.
- Cryoprecipitated Antihemophilic Factor (Cryo) is a portion of plasma rich in Specific clotting factors, including Factor VIII and fibrinogen.
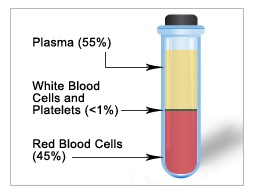
A Tube Sample of Centrifuged Blood with its Constituents
4. Blood Groups
Although all blood is made of the same basic elements, not all blood is alike. In fact, there are eight different common blood types, which are determined by the presence or absence of certain antigens – substances that can trigger an immune response if they are foreign to the body. Since some antigens can trigger a patient's immune system to attack the transfused blood, safe blood transfusions depend on careful blood typing and cross-matching.
There are four major blood groups determined by the presence or absence of two antigens – A and B – on the surface of red blood cells:
• Group A – has only the A antigen on red cells (and B antibody in the plasma)
• Group B – has only the B antigen on red cells (and A antibody in the plasma)
• Group AB – has both A and B antigens on red cells (but neither A nor B
antibodies in the plasma)
• Group O – has neither A nor B antigens on red cells (but both A and B
antibodies are in the plasma)
There are very specific ways in which blood types must be matched for a safe transfusion
In addition to the A and B antigens, there is a third antigen called the D antigen, which
can be either present (+) or absent (-). In general, D negative blood is given to D
negative patients and D positive or D negative blood may be given to Rh positive patients.
The universal red blood cell donor has the O negative blood group.
The universal plasma donor has the AB blood group.
Donor blood group
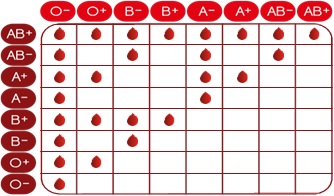
Recipient blood group
II. Blood Donation
1. Different Types of Donation
Blood is made of different components that can be removed together (whole blood donation) or separated by using a cell separator (apheresis collection).
Whole blood donation
This type of blood donation usually takes about an hour, though the actual donation takes about 8-10 minutes. Between 420 and 450 ml of blood is collected during a single donation (≤ no more than 13% of total blood volume), excluding samples for laboratory tests.
- Men can give blood up to 6 times a year, women up to 4 times a year
- Donors must be aged between 18 and 65. After the age of 60, first-time donors require the approval of a transfusion medicine physician.
- After the age of 65, blood donations are not allowed, with exceptions requiring approval of a transfusion medicine physician (for rare groups)
- Donors must wait at least 8 weeks between donations
Platelet Donations
This type of donation takes approximately 2 hours, though the actual donation takes about 70-90 minutes.
The collected blood is separated into its various components by using an apharesis machine.
The platelets are collected in a bag containing up to 650 ml (≤ 13% of the donor’s total blood volume) and the other components are returned to the donor.
This type of donation takes approximately 2 hours, though the actual donation takes about 70-90 minutes.
The collected blood is separated into its various components by using an apharesis machine.
The platelets are collected in a bag containing up to 650 ml (≤ 13% of the donor’s total blood volume) and the other components are returned to the donor.
- Each donor can give platelets up to 24 times a year
- Donors must be aged between 18 and 65. After the age of 60, first-time donors require the approval of a transfusion medicine physician
- Donors can donate every 48 hours, up to twice per week
- Donors can donate platelets between two whole blood donations
A DONOR MAY DONATE PLATELETS A MAXIMUM OF 24 TIMES A YEAR.
2. Steps of the Donation: What to Expect when you Donate Blood
Donating blood is a fairly straightforward process, but it is important to understand how it works before you begin. It can also be helpful to talk to someone you know who has donated before. The entire blood donation process takes about 45 minutes. Before you arrive to donate have something to eat and drink and make sure you get a good night’s sleep. If you are hungry or thirsty at the time of your donation, you may be at a slightly increased risk of experiencing a reaction to donating. Drink an extra 500 ml of water and other fluids before donations.
For a quick overview of the full process, watch this video.
Blood is donated in four steps:
2. Steps of the Donation: What to Expect when you Donate Blood
Donating blood is a fairly straightforward process, but it is important to understand how it works before you begin. It can also be helpful to talk to someone you know who has donated before. The entire blood donation process takes about 45 minutes. Before you arrive to donate have something to eat and drink and make sure you get a good night’s sleep. If you are hungry or thirsty at the time of your donation, you may be at a slightly increased risk of experiencing a reaction to donating. Drink an extra 500 ml of water and other fluids before donations.
For a quick overview of the full process, watch this video.
Blood is donated in four steps:
- Registration
The blood bank staff will register you and provide you with educational material (pre donation information link) that describes the donation process.
- Medical History, Vital Signs and Hemoglobin Level
In a private and confidential interview, you will be asked about your medical history and the places you have traveled to. We will take your pulse, temperature and blood pressure and screen your hemoglobin level.
- The Blood Donation
Once in the donation area, we disinfect an area on your arm to ensure the needle site is sterile. We always use a new sterile needle for every donation and safety dispose of used needles.
When we draw your blood, we keep a sample for testing and collect about 450 ml for transfusion. While your blood is being drawn, the staff monitors you and your progress to make sure you continue to feel well and there are no concerns.
After the needle is removed, sterile gauze is applied to cover the puncture site.
- Refreshments and Post Donation Care
Once you have finished donating blood, the transfusion center staff is there to ensure you are feeling alright. There is a short recovery time, about 5 minutes, during which we monitor you to make sure you have no adverse reaction to the donation. Then you will be shown to the refreshment area and given offered food and beverages.
You may resume all activities after donating blood except for the strenuous ones. The amount of blood collected is small compared to the total blood volume of an average-sized person. After donation, your body has an amazing capacity to replace all the cells and fluids that have been lost
When you leave the clinic for the rest of the day, drink plenty of fluids such as water or juice (avoid alcoholic beverages) and avoid smoking.
You may resume all activities after donating blood except for the strenuous ones. The amount of blood collected is small compared to the total blood volume of an average-sized person. After donation, your body has an amazing capacity to replace all the cells and fluids that have been lost
When you leave the clinic for the rest of the day, drink plenty of fluids such as water or juice (avoid alcoholic beverages) and avoid smoking.
3. Who Can Donate Blood ?
Donating blood is a responsible, voluntary unpaid act.
Blood Donors:
- Must be in good general health
- Must be at least 18 years old and no more than 65. After the age of 60, donors require the approval of a transfusion medicine physician
- Must weight at least 50 kg
- Must not be at risk of transmitting blood-borne diseases
- Must have a hemoglobin or hematocrit level of:
o 13.5-18 g/dl (0.40%) for a man
o 12.5-16 g/dl (0.38%) for a woman
o 12.5-16 g/dl (0.38%) for a woman
- Must have a systolic blood pressure of 100-140 mmHg and a diastolic blood pressure of 60-90 mmHg
- Must have a pulse rate of 60-100 bpm (beats per minute)
- Must have a temperature below 37.6°C
- Must have a platelet count above 150x109/L
You should not donate blood if:
- You have ever taken drugs
- Your partner takes drugs
- You are HIV positive
- You are a male who had sexual contacts with another male
- Your partner is HIV positive
- You have more than one sexual partner
- You think your partner has risky sex
These instructions must be strictly respected even when using a condom.
Wait 6 months before donation if:
Wait 6 months before donation if:
- You have casual partners
- You have changed sexual partners
These instructions must be strictly respected even when using a condom.
Wait 12 months before donation:
Wait 12 months before donation:
- after a tattoo or ear/body piercing
- after a scarification (except if therapeutic)
- if you have undergone an acupuncture treatment and did not have needles for strictly personal use or single-use needles
- if you have been cut with potentially contaminated objects (through sharing razor blades, for example)
- if you have had prolonged contact with a damaged skin contaminated with secretions or blood
- if you have been injured with a dirty needle
- In case of a human bite
- After surgery or endoscopic evaluation
Blood transfusion safety depends on the strict respect of these instructions for preventing transmission of blood-borne HIV or other infections.
4. What Happens to your Blood Donation ?
A process is in place at all blood banks to assure a safe blood collection from the donor, quality testing and processing, safe administration to the patient.
4. What Happens to your Blood Donation ?
A process is in place at all blood banks to assure a safe blood collection from the donor, quality testing and processing, safe administration to the patient.
- Blood Collection
Before donating blood the donor fills out a questionnaire to determine his/her eligibility on that specific day. To be accepted for blood donation, prospective blood donors should feel healthy and well on the day of donation and must meet all requirements and criteria defined by the donor centers.
- Processing
Blood is processed in order to prepare the blood component that the patient needs. Prior to processing into blood components, the white blood cells (also known as leukocytes) are filtered out to reduce the risk of a transfusion reaction. Since January 2013, Blood Banks in Lebanon perform leukocyte reduction.
- Tests
The blood samples collected during the donation are sent to the testing laboratory to determine the donor’s blood type and screen for infections such as hepatitis B and C, syphilis and HIV. If a test returns positive the blood unit is destroyed and the donor is notified.
- Distribution
III. Public Information and Brochures
- Brochures:
II.Information For The Health Professionals
I. Lebanese Committee of Blood Transfusion
1. Introduction
All activities related with blood collection, biological qualification of labile blood products, blood processing, storage and distribution, must be coordinated at the national level, through effective organization and national blood policy. These must be governed by appropriate legislation framework to promote uniform implementation of standards and consistency in quality and safety of blood and blood products.
2. Who Are We?
The national policy in blood transfusion is implemented and monitored by the ministry of public health in Lebanon, based on the official committee’s recommendations: the Lebanese National Committee of Blood Transfusion (LNCBT)
3. Mission
The Lebanese NCBT public service mission is to provide advice to the ministry on:
All activities related with blood collection, biological qualification of labile blood products, blood processing, storage and distribution, must be coordinated at the national level, through effective organization and national blood policy. These must be governed by appropriate legislation framework to promote uniform implementation of standards and consistency in quality and safety of blood and blood products.
2. Who Are We?
The national policy in blood transfusion is implemented and monitored by the ministry of public health in Lebanon, based on the official committee’s recommendations: the Lebanese National Committee of Blood Transfusion (LNCBT)
3. Mission
The Lebanese NCBT public service mission is to provide advice to the ministry on:
- The organization of blood policy
- The development of strategies and measures for policies, planning, and legal structuring (legal framework, logistical and staff support) of national self-sufficiency technical issues
- The promotion of voluntary anonymous unpaid blood donation
- Training on blood transfusion for medical and paramedical staff
- The improvement and sharing of transfusion practices
- The dissemination of technical guidelines for good practices and quality assurance in blood transfusion
- The development and organization of a haemovigilance system at the national level
- Data centralizing and processing
- The assessment of the country’s potential need for blood to ensure that a sufficient supply of blood products is available.
4. Contact Us
II. National Blood Strategy
National Policy and Strategic Framework for Blood Transfusion Services in Lebanon- February 2022
III. Blood Donation
1. Different Types of Donation
Blood is made of different components that can be removed together (whole blood donation) or separated by using a cell separator (apheresis collection).
Whole blood donation
This type of blood donation usually takes about an hour, though the actual donation takes about 8-10 minutes. Between 420 and 450 ml of blood is collected during a single donation (≤ no more than 13% of total blood volume), excluding samples for laboratory tests.
- Men can give blood up to 6 times a year, women up to 4 times a year
- Donors must be aged between 18 and 65. After the age of 60, first-time donors require the approval of a transfusion medicine physician.
- After the age of 65, blood donations are not allowed, with exceptions requiring approval of a transfusion medicine physician (for rare groups)
- Donors must wait at least 8 weeks between donations
Platelet Donations
This type of donation takes approximately 2 hours, though the actual donation takes about 70-90 minutes.
The collected blood is separated into its various components by using an apharesis machine.
The platelets are collected in a bag containing up to 650 ml (≤ 13% of the donor’s total blood volume) and the other components are returned to the donor.
This type of donation takes approximately 2 hours, though the actual donation takes about 70-90 minutes.
The collected blood is separated into its various components by using an apharesis machine.
The platelets are collected in a bag containing up to 650 ml (≤ 13% of the donor’s total blood volume) and the other components are returned to the donor.
- Each donor can give platelets up to 24 times a year
- Donors must be aged between 18 and 65. After the age of 60, first-time donors require the approval of a transfusion medicine physician
- Donors can donate every 48 hours, up to twice per week
- Donors can donate platelets between two whole blood donations
A DONOR MAY DONATE PLATELETS A MAXIMUM OF 24 TIMES A YEAR.
2. Steps of the Donation: What to Expect when you Donate Blood
Donating blood is a fairly straightforward process, but it is important to understand how it works before you begin. It can also be helpful to talk to someone you know who has donated before. The entire blood donation process takes about 45 minutes. Before you arrive to donate have something to eat and drink and make sure you get a good night’s sleep. If you are hungry or thirsty at the time of your donation, you may be at a slightly increased risk of experiencing a reaction to donating. Drink an extra 500 ml of water and other fluids before donations.
For a quick overview of the full process, watch this video.
Blood is donated in four steps:
2. Steps of the Donation: What to Expect when you Donate Blood
Donating blood is a fairly straightforward process, but it is important to understand how it works before you begin. It can also be helpful to talk to someone you know who has donated before. The entire blood donation process takes about 45 minutes. Before you arrive to donate have something to eat and drink and make sure you get a good night’s sleep. If you are hungry or thirsty at the time of your donation, you may be at a slightly increased risk of experiencing a reaction to donating. Drink an extra 500 ml of water and other fluids before donations.
For a quick overview of the full process, watch this video.
Blood is donated in four steps:
- Registration
The blood bank staff will register you and provide you with educational material (pre donation information link) that describes the donation process.
- Medical History, Vital Signs and Hemoglobin Level
In a private and confidential interview, you will be asked about your medical history and the places you have traveled to. We will take your pulse, temperature and blood pressure and screen your hemoglobin level.
- The Blood Donation
Once in the donation area, we disinfect an area on your arm to ensure the needle site is sterile. We always use a new sterile needle for every donation and safety dispose of used needles.
When we draw your blood, we keep a sample for testing and collect about 450 ml for transfusion. While your blood is being drawn, the staff monitors you and your progress to make sure you continue to feel well and there are no concerns.
After the needle is removed, sterile gauze is applied to cover the puncture site.
- Refreshments and Post Donation Care
Once you have finished donating blood, the transfusion center staff is there to ensure you are feeling alright. There is a short recovery time, about 5 minutes, during which we monitor you to make sure you have no adverse reaction to the donation. Then you will be shown to the refreshment area and given offered food and beverages.
You may resume all activities after donating blood except for the strenuous ones. The amount of blood collected is small compared to the total blood volume of an average-sized person. After donation, your body has an amazing capacity to replace all the cells and fluids that have been lost
When you leave the clinic for the rest of the day, drink plenty of fluids such as water or juice (avoid alcoholic beverages) and avoid smoking.
You may resume all activities after donating blood except for the strenuous ones. The amount of blood collected is small compared to the total blood volume of an average-sized person. After donation, your body has an amazing capacity to replace all the cells and fluids that have been lost
When you leave the clinic for the rest of the day, drink plenty of fluids such as water or juice (avoid alcoholic beverages) and avoid smoking.
3. Who Can Donate Blood ?
Donating blood is a responsible, voluntary unpaid act.
Blood Donors:
- Must be in good general health
- Must be at least 18 years old and no more than 65. After the age of 60, donors require the approval of a transfusion medicine physician
- Must weight at least 50 kg
- Must not be at risk of transmitting blood-borne diseases
- Must have a hemoglobin or hematocrit level of:
o 13.5-18 g/dl (0.40%) for a man
o 12.5-16 g/dl (0.38%) for a woman
o 12.5-16 g/dl (0.38%) for a woman
- Must have a systolic blood pressure of 100-140 mmHg and a diastolic blood pressure of 60-90 mmHg
- Must have a pulse rate of 60-100 bpm (beats per minute)
- Must have a temperature below 37.6°C
- Must have a platelet count above 150x109/L
You should not donate blood if:
- You have ever taken drugs
- Your partner takes drugs
- You are HIV positive
- You are a male who had sexual contacts with another male
- Your partner is HIV positive
- You have more than one sexual partner
- You think your partner has risky sex
These instructions must be strictly respected even when using a condom.
Wait 6 months before donation if:
Wait 6 months before donation if:
- You have casual partners
- You have changed sexual partners
These instructions must be strictly respected even when using a condom.
Wait 12 months before donation:
Wait 12 months before donation:
- after a tattoo or ear/body piercing
- after a scarification (except if therapeutic)
- if you have undergone an acupuncture treatment and did not have needles for strictly personal use or single-use needles
- if you have been cut with potentially contaminated objects (through sharing razor blades, for example)
- if you have had prolonged contact with a damaged skin contaminated with secretions or blood
- if you have been injured with a dirty needle
- In case of a human bite
- After surgery or endoscopic evaluation
Blood transfusion safety depends on the strict respect of these instructions for preventing transmission of blood-borne HIV or other infections.
4. What Happens to your Blood Donation ?
A process is in place at all blood banks to assure a safe blood collection from the donor, quality testing and processing, safe administration to the patient.
4. What Happens to your Blood Donation ?
A process is in place at all blood banks to assure a safe blood collection from the donor, quality testing and processing, safe administration to the patient.
- Blood Collection
Before donating blood the donor fills out a questionnaire to determine his/her eligibility on that specific day. To be accepted for blood donation, prospective blood donors should feel healthy and well on the day of donation and must meet all requirements and criteria defined by the donor centers.
- Processing
Blood is processed in order to prepare the blood component that the patient needs. Prior to processing into blood components, the white blood cells (also known as leukocytes) are filtered out to reduce the risk of a transfusion reaction. Since January 2013, Blood Banks in Lebanon perform leukocyte reduction.
- Tests
The blood samples collected during the donation are sent to the testing laboratory to determine the donor’s blood type and screen for infections such as hepatitis B and C, syphilis and HIV. If a test returns positive the blood unit is destroyed and the donor is notified.
- Distribution
The blood product is released to the patient after the donor-recipient compatibility tests are completed and the blood component is documented safe and compatible.
A. Procedures:
IV. Regulatory Framework and Good Transfusion Practices
- Principles of Good Transfusion Practices
- Good practices in the Transport of Blood/Blood Products and Blood Samples
- Ministerial Decrees on Blood Transfusion
English
French
Arabic
French
Arabic
V. National Procedures and Specifications
A. Procedures:
- Blood Collection:
- 1. Whole Blood Donor Questionnaire
- 5. Brochures
- Blood Testing:
- 1. Good laboratory practices in red cell immunohematology
- 2. Blood donation testing reagents
- 3.Decisional Algorithms for testing Blood Donations
- 4. Course of action for abnormal test results in blood donors
- 5.Technical procedures for implementing the infectious disease screening tests
- Preparation:
- 1.List of blood components
VI. Hemovigilance
- The Organizational Aspect of Hemovigilance in Lebanon
- Manual for Data Entry on the Platform
- Transfusion Reaction report - The Recipient (HV 002)
- Guide d'Utilisation (HV 003)
English
French
French
- List and codes of adverse Transfusion reactions for the recipient (HV 004)
- HV FEIGD 005
English
French
French
- List and Codification of Serious Adverse Reactions Donor ( HV 006)
- Annual Hemovigilance Activity Report (HV 008)
VII. National Standards for Qualification of Blood Banks
- Standards for good transfusion practice guidelines
VIII. Forms and Templates
- Agreements between Transfusion Centers :
English
French
Arabic
French
Arabic
- Transfusion Informed Consent
IX. Activities and Events
X. News and Updates
XI. References and Links
Contact us
Sitemap 

© Copyrights reserved to Ministry of Public Health 2026






